How AI Medical Scribes Work Inside Your EHR (Step-by-Step Workflow)

Healthcare providers today are spending a significant portion of their time on documentation rather than patient care. Managing electronic health records (EHRs), completing clinical notes, and ensuring compliance often extends beyond working hours, adding to daily pressure and fatigue.
Across the United States, many clinics are now adopting HIPAA-compliant AI medical scribe services to reduce this burden. By automating documentation and integrating directly into EHR systems, these solutions help providers save time while maintaining accuracy and compliance.
What Is an AI Medical Scribe?
An AI medical scribe is a technology solution designed to capture and convert doctor–patient interactions into structured clinical documentation. Unlike traditional dictation tools, it does more than just transcribe speech.
It understands clinical context, extracts relevant medical details, and organizes them into structured formats such as SOAP notes. This allows healthcare providers to focus on patient care while the documentation process happens in the background.
Step-by-Step Workflow:
How AI Medical Scribes Work
Pre-Charting Before the Visit
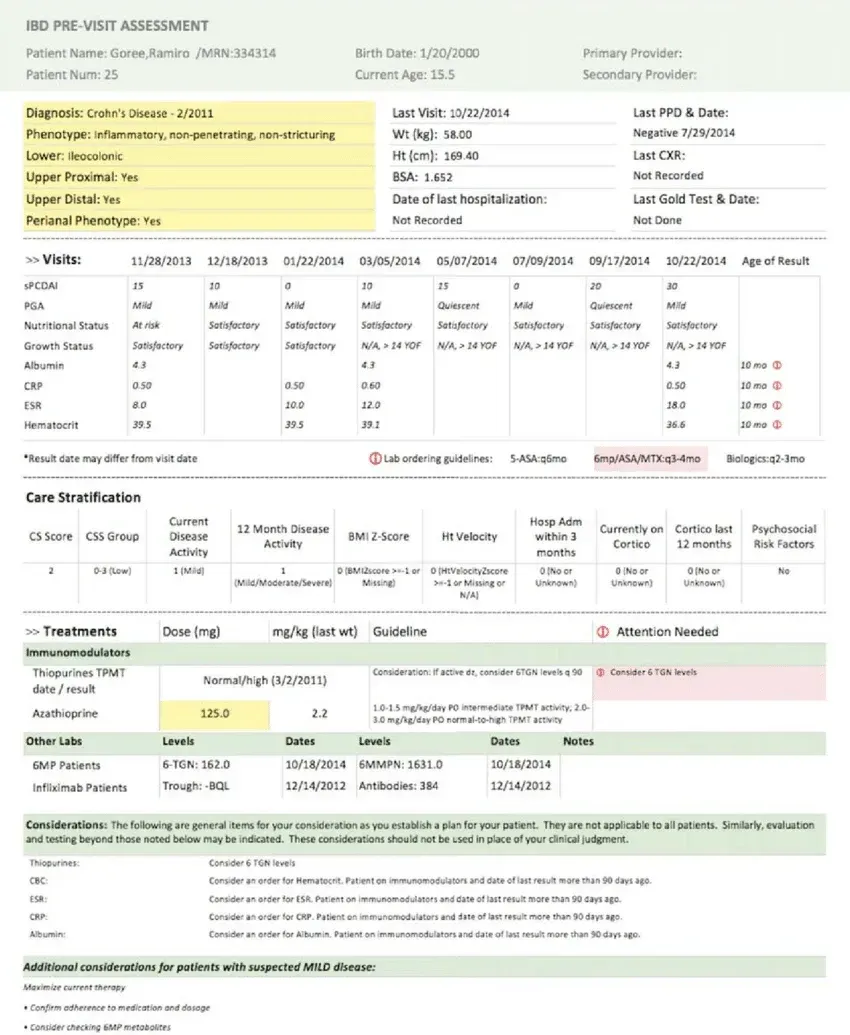
Before the patient visit begins, the pre-charting process prepares the foundation for accurate documentation. The system reviews existing patient records, including prior visit notes, medications, allergies, lab results, and any recent updates available in the EHR.
Relevant details are organized into a structured format so the provider starts the visit with clear clinical context. This may include highlighting gaps in documentation, pending lab results, or follow-up items from previous encounters.
By doing this in advance, the provider avoids switching between screens during the consultation and can focus entirely on patient interaction while the system already understands the background.
Patient Encounter Begins
During the clinical visit, ambient clinical intelligence works passively in the background, capturing the conversation in a natural, unobtrusive way. The provider does not need to change their behavior or use commands—the system listens and processes in real time.
It intelligently identifies speakers and captures relevant inputs not only from the patient but also from accompanying individuals. For example, in pediatric visits, parents often provide key medical history, while in other cases, caregivers or family members contribute important details.
The AI distinguishes clinically relevant information such as symptoms, timelines, and concerns—from casual conversation. This ensures that meaningful context is captured accurately without adding unnecessary content to the record.
Real-Time Transcription
As the interaction continues, the system converts speech into text instantly. Unlike basic dictation tools, it understands medical vocabulary, abbreviations, and conversational phrasing commonly used in clinical settings.
It also adapts to different speaking styles, accents, and multi-speaker environments. Background noise or unrelated discussion is filtered out to maintain clarity.
The result is a clean, accurate transcript that reflects the full clinical conversation without requiring manual correction.

Clinical Structuring and Understanding
After transcription, the AI analyzes the content to extract and organize clinical data. It identifies key components such as chief complaint, history of present illness (HPI), review of systems (ROS), assessment, and plan.
The system applies clinical logic to structure the information appropriately for example, separating subjective and objective findings or aligning symptoms with timelines.
It also ensures consistency in terminology and formatting, which supports better readability, coding accuracy, and compliance.
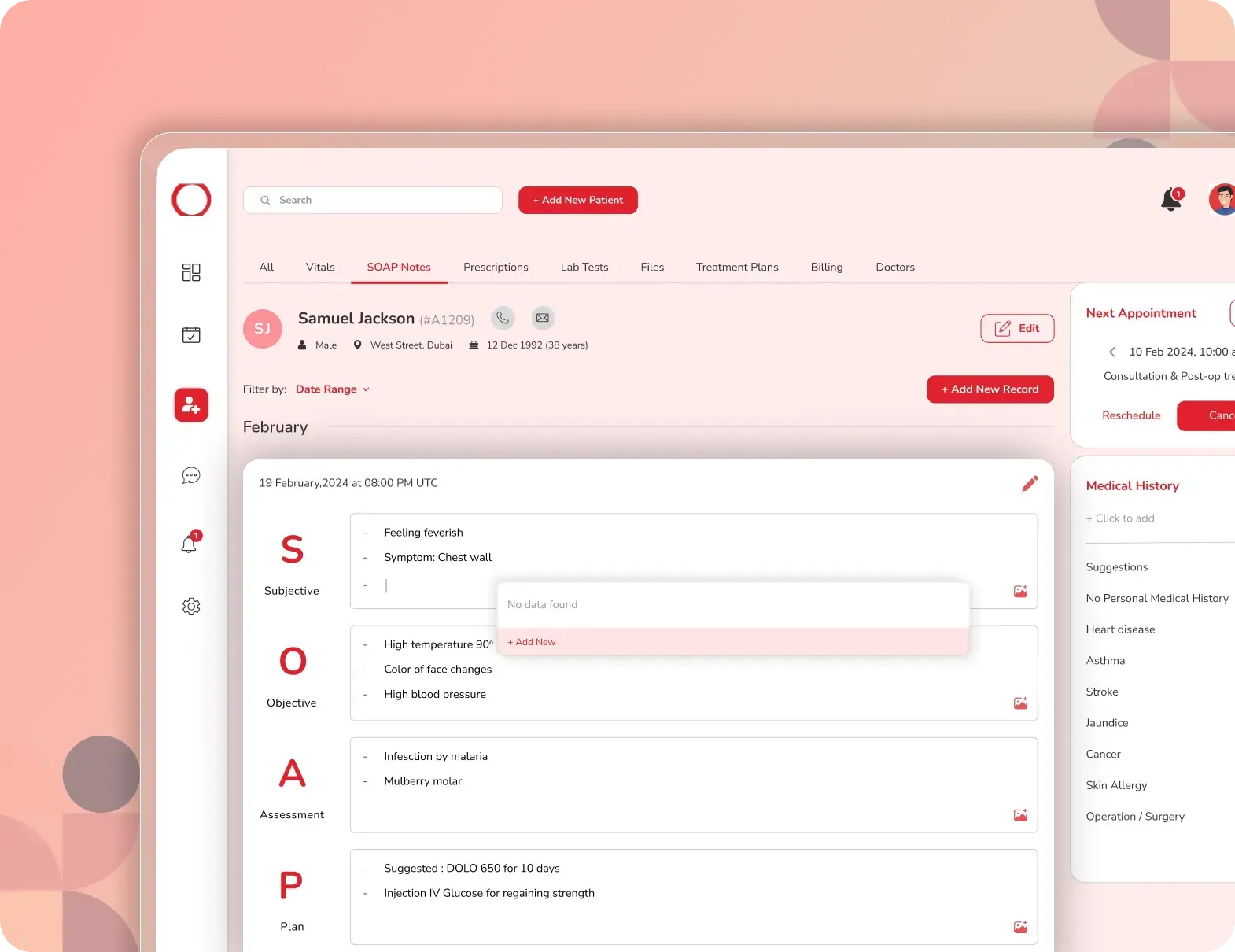
Auto-Generated Clinical Notes
Using the structured data, the AI generates a complete clinical note with completely incorporated Pre-chart tailored to the provider’s preferred format. This can include SOAP notes, progress notes, Admission notes or specialty-specific templates.
The notes are not just transcripts they are refined, clinically relevant documents that align with documentation standards. Redundant or irrelevant content is removed, and key medical details are clearly presented.
This step significantly reduces the need for manual typing while maintaining high-quality documentation with ICD-10 codes.
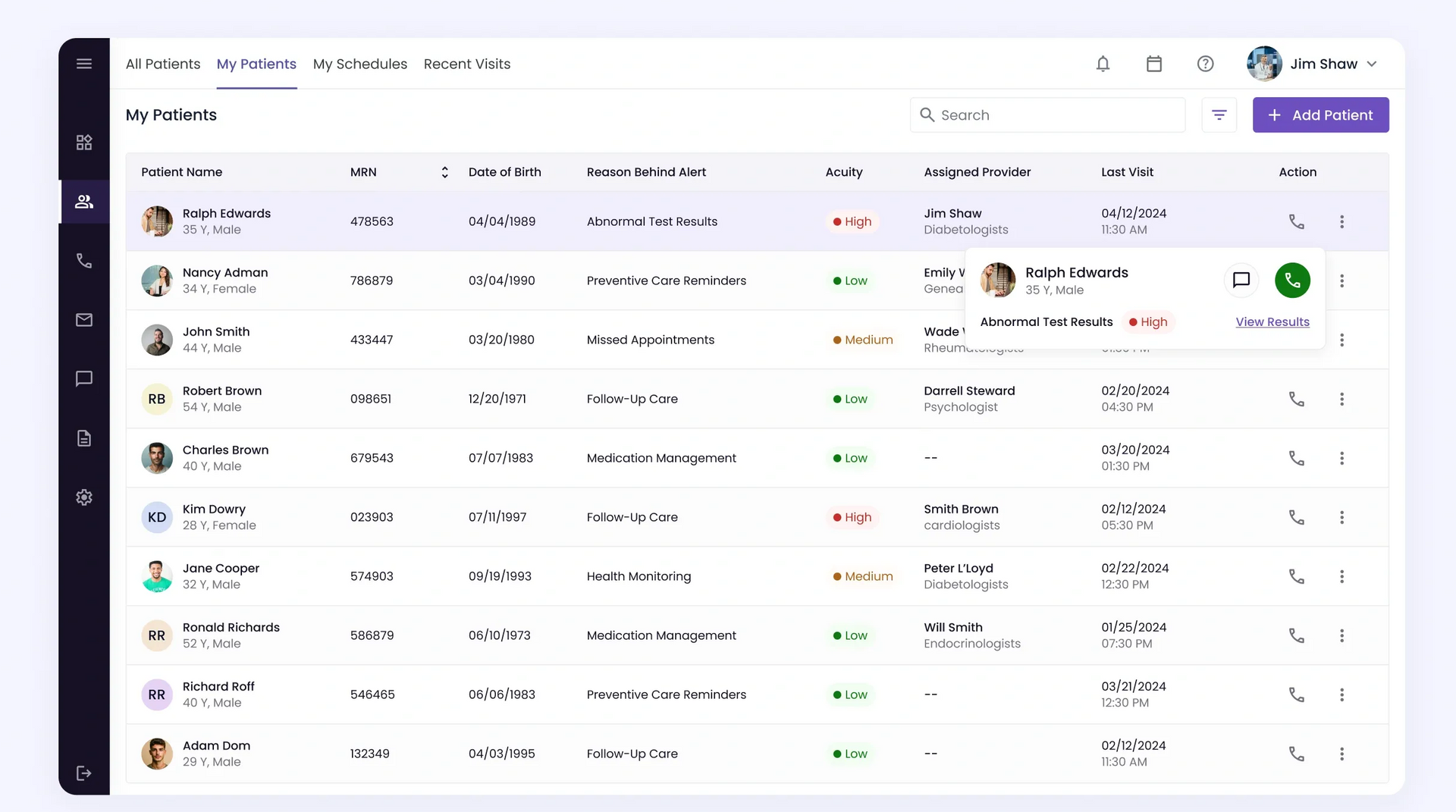
Physician Review and Finalization
The physician then reviews the generated note within the EHR. If any information is missing or needs clarification, additional details can be dictated naturally and added to the note without disrupting the workflow.
This stage also supports flexibility. If the provider is waiting for lab results, imaging reports, or additional patient information, the note can be paused and saved in progress. Once the required data becomes available, the provider can resume, incorporate the new details, and finalize the documentation.
This eliminates the need to recreate notes and ensures completeness without time pressure.

Seamless Integration into the EHR
Once finalized, the note is automatically integrated into the EHR system in the correct patient record. There is no need for manual copying, uploading, or formatting adjustments.
The documentation is immediately available for clinical reference, billing, coding, and compliance purposes. This seamless integration reduces administrative effort and minimizes the risk of errors or missing information.
HIPAA-Compliant
AI Medical Scribe Services
Data security is a critical concern in healthcare. AI medical scribe solutions are designed to comply with HIPAA regulations, ensuring that patient information is handled securely and confidentially.
These systems use encrypted processing and secure access controls to protect sensitive data. This makes them suitable for clinics operating in regulated environments, including practices in major healthcare hubs like New York.
Benefits of AI Medical Scribes in EHR Workflow
AI medical scribes help reduce the time spent on documentation, allowing providers to focus more on patient care. This leads to better patient interactions and improved satisfaction.
They also reduce after-hours charting, helping to minimize burnout. In addition, structured documentation improves accuracy and supports better coding and compliance, which is essential for efficient practice management.
Are AI Medical Scribes Fully Automated?
While AI medical scribes are highly advanced, they are not completely independent. Most effective solutions combine AI with human oversight to ensure accuracy and quality.
This approach allows providers to benefit from automation while maintaining control over their documentation.
Who Can Benefit the Most?
AI medical scribes are ideal for healthcare providers who manage high patient volumes or complex documentation. This includes primary care physicians, specialists, and telehealth providers.
Any practice looking to reduce administrative workload and improve efficiency can benefit from adopting this technology.
Conclusion
AI medical scribes are transforming clinical documentation by simplifying workflows and reducing the burden on healthcare providers. By integrating directly into EHR systems, they automate one of the most time-consuming tasks in healthcare.
For clinics looking to improve efficiency and reduce documentation stress, AI medical scribes offer a practical and effective solution.
If your clinic is looking to reduce documentation time and improve workflow efficiency, HIPAA-compliant AI medical scribe services can help.
Request a demo today and experience a smarter way to manage clinical documentation.
Optional
FAQ
How much time can doctors save using AI medical scribes?
Doctors can save several hours each day by reducing manual documentation and after-hours charting, allowing more focus on patient care.
Are AI medical scribes suitable for small clinics?
Yes, AI medical scribes are ideal for both small clinics and large healthcare organizations. They help reduce workload without requiring additional staff.
What types of notes can AI medical scribes generate?
They can generate various clinical notes, including SOAP notes, progress notes, history of present illness (HPI), and discharge summaries.
How does Chase’s AI medical scribe fit into my current workflow?
Our AI medical scribe works alongside your existing workflow by capturing patient conversations and automatically generating structured notes directly within your EHR, with minimal disruption.
Will I need to change my EHR system to use your service?
No, our solution is designed to integrate with most EHR systems. We adapt to your setup, so you don’t need to switch platforms or change how you work.
Can I customize how my notes are formatted?
Absolutely. We offer customized documentation formats based on your preferences, including SOAP notes, templates, and provider-specific styles.
How quickly can I get started with Chase Clinical Documentation?
You can get started quickly with our streamlined onboarding process. Once set up, you can begin using the service almost immediately.
Recent Posts










